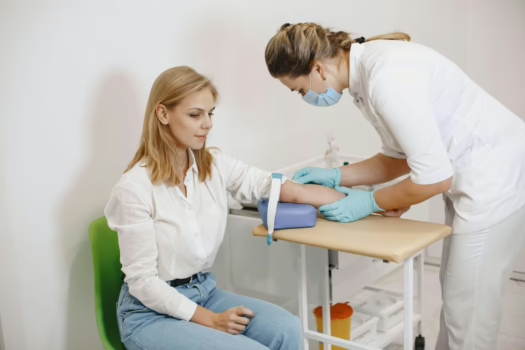
Most nurses remember the shift when the thought first creeps in. It is usually late in the day, after handling several complicated patients, when you realize you are already guiding most of the care decisions but still need someone else to formally approve them.
That moment has become common across hospitals and clinics. Experienced nurses carry a large part of the clinical thinking behind patient care. Moving into advanced practice can feel like the logical next step. Still, the change is not as straightforward as starting graduate school and waiting for a new title. The role shifts in ways that only become clear once you step into it.
The Responsibility Shift That Comes with Advanced Practice
One of the first differences nurses notice in advanced roles is how responsibility moves. At the bedside, nurses already manage complex care, but the final call on diagnosis or treatment usually belongs to someone else. In advanced practice, those decisions begin to rest with you.
That change can feel rewarding and a little heavy at the same time. Nurse practitioners and other advanced providers evaluate symptoms, review tests, and decide on treatment plans with far less supervision. Education prepares nurses for the role, but the adjustment still takes time. Early months often feel like a steep learning curve while confidence slowly catches up with the new level of responsibility.
Understanding the Financial Side of the Career Move
For many nurses, financial considerations play at least some role in the decision to pursue advanced education. Graduate programs require both time and money, and stepping away from full-time work during training can add pressure.
Advanced practice roles do tend to offer stronger earning potential over time. For instance, AGPCNP salary would be higher than that of a nurse who hasn’t pursued advanced education. Salaries vary depending on specialty, geographic region, and type of healthcare facility, but compensation usually reflects the added responsibility and clinical authority. Looking at realistic salary ranges helps many nurses weigh the cost of graduate education against future income and career stability. The financial picture is rarely the only factor in the decision, but it is one that deserves honest consideration before beginning the transition.
Education Is Only Part of the Transition
Graduate education is the most visible step toward advanced practice, yet the learning process rarely ends with a degree. Programs provide the clinical knowledge and licensing requirements needed to practice, but the everyday realities of the role continue to develop afterward.
New nurse practitioners often describe their first year as a second round of training. Clinical judgment becomes sharper through repetition. Patterns in patient care begin to appear more clearly. Communication with physicians, specialists, and healthcare administrators also takes on new importance.
Healthcare environments are complex, and advanced practice providers often sit in the middle of several different systems. They coordinate care, interpret medical data, and translate information for patients who may feel overwhelmed by medical terminology. This broader role can feel rewarding, but it also requires patience while experience catches up with education.
The Relationship with Patients Changes
One subtle shift in advanced practice is the way patient relationships evolve. Bedside nurses spend a great deal of time with patients, often becoming the primary source of comfort during stressful hospital stays. That connection remains valuable, but the dynamic changes slightly.
In advanced roles, patients often view the provider as the person responsible for diagnosis and treatment planning. Conversations may focus more on medical decisions and long-term care strategies rather than moment-to-moment support.
That does not remove the human side of the profession. Many nurse practitioners maintain a patient-centered approach that blends clinical authority with the empathy developed during years of bedside nursing. Still, the conversations tend to become more structured and focused on decision-making.
Workplace Expectations Can Shift
Another change that sometimes surprises new advanced practitioners involves workplace expectations. Healthcare organizations often rely heavily on nurse practitioners to expand access to care, especially in primary care environments where physician shortages are common. As a result, patient schedules may become quite full. Clinics aim to serve as many people as possible while maintaining quality care, which means advanced practice providers often manage significant patient loads.
Time management becomes an essential skill. Charting, patient follow-ups, and coordination with specialists can easily extend beyond scheduled clinic hours if routines are not carefully organized. Experienced nurses usually adapt well to this environment because they are already accustomed to busy clinical settings. Still, the administrative responsibilities in advanced practice can feel heavier than expected.
Professional Identity Evolves Over Time
One topic that rarely appears in program brochures is the shift in professional identity that comes with advanced practice roles. Nurses entering graduate programs often carry a strong connection to bedside care, teamwork, and the traditional nursing model. As advanced practitioners, they begin to occupy a hybrid position within the healthcare system. They remain grounded in nursing philosophy while also functioning as independent clinical providers.
Some nurses experience a brief period of uncertainty during this transition. They may wonder where they fit within the clinical hierarchy or how their role differs from that of physicians and other healthcare professionals. Over time, that uncertainty tends to fade. Most advanced practice nurses develop a clear sense of their contribution to patient care, often bridging the gap between medical decision-making and compassionate communication.
The Decision Requires Honest Reflection
Moving into advanced practice is rarely a decision made lightly. Graduate programs demand commitment, and the clinical responsibilities that follow require confidence and adaptability.
For nurses considering the step, the most helpful starting point is honest reflection. Why pursue advanced practice? Is the motivation rooted in a desire for deeper clinical involvement, long-term career growth, or broader influence in patient care? There is no single correct answer. Many nurses pursue advanced roles for a combination of reasons that evolve over time.
What matters most is understanding that the transition changes more than a job title. It reshapes daily responsibilities, professional relationships, and the scope of clinical decision-making. Those who enter the field with realistic expectations often find that the role brings both challenges and a deep sense of professional satisfaction. The path requires patience, but for many nurses, it becomes the natural continuation of a career built on caring for patients and improving the healthcare system around them.
Follow me down the rabbit hole!
I'm Alice and I live with a dizzying assortment of invisible disabilities, including ADHD and fibromyalgia. I write to raise awareness and end the stigma surrounding mental and chronic illnesses of all kinds.