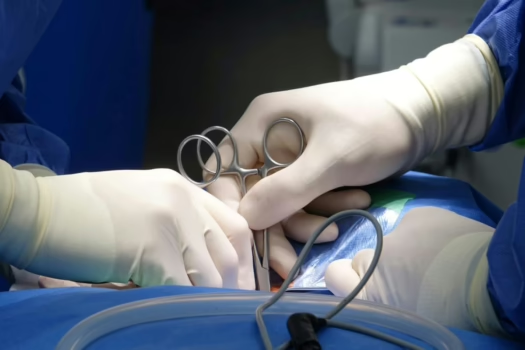
Surgical mistakes can turn minimal-risk, routine procedures into life-altering events. These errors are often preventable, yet remain a leading cause of medical malpractice claims in the U.S. Early documentation, expert opinions, and careful timing often determine whether a case succeeds.
These errors, sometimes called “never events,” account for a significant portion of malpractice payouts nationwide. Acting promptly and understanding what counts as negligence can make the difference between a strong settlement and a denied claim.
If you’ve been harmed by a surgical mistake, knowing your rights and how claims work is important. Many claims require showing that the surgeon failed to meet the standard of care and that this directly caused your injury. Working with a skilled surgical error attorney can help you collect evidence, establish liability, and maximize your chances of fair compensation.
What are Some Common Surgical Errors That Lead to Malpractice Claims?
Here are some common surgical mistakes that happen more frequently than others:
- Wrong-site or wrong-procedure surgery – Occurs due to miscommunication or verification failures. Studies report roughly 40 incidents weekly nationwide.
- Retained Foreign Objects – Instruments or sponges left inside patients happen in up to 1 in 1,000 abdominal surgeries.
- Anesthesia Complications and Unintended Organ or Nerve Damage – Affect more than one in three surgical patients with complications linked to errors.
These errors are considered preventable under the Joint Commission’s Universal Protocol, which requires pre-op “time-outs” for site verification, patient ID, and procedure confirmation. Hospitals that fail to follow CMS Conditions of Participation (42 CFR § 482.41) might be liable for systemic negligence.
Proving Medical Malpractice
To succeed in a surgical error claim, four elements must be established: duty, breach, causation, and damages, as outlined under state tort law and common law principles.
Expert testimony is key. Board-certified surgeons or specialists confirm whether the standard of care was breached and if that breach directly caused injury. Medical errors rank as the third leading cause of death in the U.S., making these claims both common and high-stakes.
State laws affect timing and damages. Statutes of limitations range from 1-3 years, while many states impose caps on non-economic damages. For instance, California’s MICRA law (Civ. Proc. Code § 3333.2) limits non-economic awards to $250K.
Prompt action post-surgery preserves evidence and strengthens your case.
Legal Recourse and Typical Outcomes
Victims can recover compensation for:
- Medical expenses and follow-up care
- Lost wages or future earning capacity
- Pain and suffering
Average settlements exceed $400K, while severe injuries like paralysis or death can push awards into the millions, even after caps.
Hospitals may face vicarious or enterprise liability, and surgeons risk license suspension or sanctions from state boards. Contingency attorneys typically advance costs and recover fees only from successful outcomes.
Discovery tools like subpoenas for OR logs, patient charts, and team depositions ensure full access to evidence. In some states, doctrines like res ipsa loquitur shift the burden to defendants in clear-cut surgical errors.
Overlooked Regulatory Safeguards
Despite oversight from FDA device regulations (21 CFR Part 820) and hospital protocols, mistakes still occur. Anesthesia dosing errors, equipment malfunctions, or mislabeling of surgical instruments are frequent sources of claims.
Following established safety protocols and documenting deviations can make or break a case.
Final Takeaways
- Surgical errors are preventable but remain a leading cause of malpractice claims.
- Wrong-site surgery, retained objects, and anesthesia mistakes are most common.
- Legal claims require proving duty, breach, causation, and damages.
- Expert testimony and proper documentation strengthen cases.
- State laws and caps may limit recovery despite serious harm.
- Contingency attorneys can help pursue compensation without upfront costs.
- Prompt action post-surgery preserves evidence and maximizes settlement potential.
Follow me down the rabbit hole!
I'm Alice and I live with a dizzying assortment of invisible disabilities, including ADHD and fibromyalgia. I write to raise awareness and end the stigma surrounding mental and chronic illnesses of all kinds.