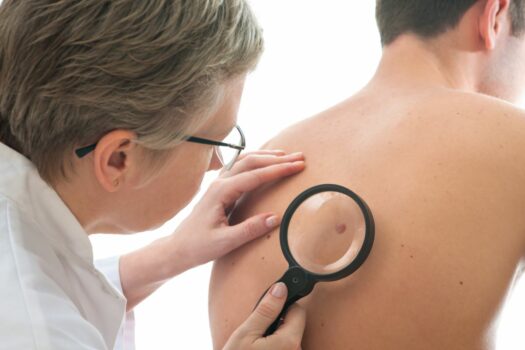
Introduction to Non-Melanoma Skin Cancer
When the topic of skin cancer arises, most of us immediately envision those ominous, dark, irregularly shaped moles that are the hallmark of melanoma. This particular form of skin cancer, while indeed dangerous, often overshadows its non-melanoma counterparts in public consciousness. The reality, though, is that many skin cancer cases aren’t melanomas at all. They belong to a category referred to as non-melanoma skin cancers. This raises an essential question: if they aren’t the classic, often-discussed melanomas, then what are they?
These non-melanoma variants can appear in various forms, spots, and colors on our skin, making them less straightforward to identify. Their nature and potential risks, however, are just as critical to understand. These types of cancers are actually more prevalent than melanomas, emphasizing the need for greater public awareness and education.
What is non-melanoma skin cancer?
Diving deep into the topic of non-melanoma skin cancers, it’s vital to pinpoint what makes them distinct. The central differentiation lies in their origin: they don’t arise from melanocytes. For those scratching their heads, melanocytes are the cells nestled within the deeper strata of our skin, with the primary job of producing melanin. This melanin not only bestows our skin, hair, and eyes with their unique shades but also acts as our natural shield, fending off the sun’s damaging ultraviolet (UV) rays.
Beneath the non-melanoma umbrella, two predominant variants stand out. Both, typically a consequence of extended exposure to sun or UV light, exhibit distinct attributes and potential complications. Grasping their nature is instrumental in early detection, timely intervention, and perhaps, sidestepping the ailment altogether.
Embarking on this voyage of comprehending non-melanoma skin cancer is pivotal. It not only accentuates the need to be alert to melanoma indicators but also highlights the vast spectrum of skin malignancies that might besiege individuals. As we widen our understanding, we equip ourselves to be proactive, ensuring timely prevention, detection, and curative measures.
Causes and Risk Factors
The inception of skin cancers, particularly the non-melanoma type, is often multifaceted, with various factors playing pivotal roles. Foremost among these is the exposure to ultraviolet (UV) radiation. This radiation is emitted in abundance by the sun. Sun-lovers, especially those without adequate protection, stand at a heightened risk. But it’s not just natural sunlight; tanning beds, often mistakenly believed to be a safer alternative to achieve that golden glow, emit concentrated UV radiation, further raising the stakes.
While UV radiation is a major player, it isn’t the sole offender. A weakened immune system can also escalate the risk. Think of the immune system as the body’s surveillance system. When it’s compromised—whether due to medical conditions, treatments, or certain medications—our ability to fend off potential cancerous changes in the skin diminishes.
But the list doesn’t end here. Prolonged exposure to specific chemicals, especially those encountered in particular industrial settings, can act as catalysts. These chemicals may include arsenic, coal tar, and certain types of oil. Furthermore, a history of radiation treatments, often administered for other health conditions, can inadvertently increase one’s vulnerability to non-melanoma skin cancers. Being aware of these risk factors can guide preventive strategies and routine check-ups, fostering early detection and treatment.
Treatment Options for Non-Melanoma Skin Cancer
When confronted with a diagnosis of non-melanoma skin cancer, the subsequent step is to chart out a tailored treatment plan. This plan, however, isn’t a one-size-fits-all approach. Instead, it’s a customized blueprint, intricately designed to cater to the specific nature of the cancer and the individual nuances of the patient.
The type of non-melanoma skin cancer is a significant determinant. Basal cell carcinomas might require a different therapeutic approach compared to squamous cell carcinomas. Size is another crucial consideration. A small, localized tumor may be dealt with differently than a more extensive, invasive one.
Location also weighs heavily in the decision-making process. A cancerous spot on the face, given its aesthetic and functional importance, might necessitate a more conservative surgical approach than one on the back.
Last, but certainly not least, the patient’s overall health plays a decisive role. Factors like age, underlying medical conditions, and the patient’s ability to tolerate certain treatments can greatly influence the chosen path.
Common treatment modalities include surgical removal (often done for localized tumors), Mohs surgery (especially useful for cancers on the face or other sensitive areas), cryotherapy, topical treatments, radiation therapy, and even laser treatments. However, the ultimate choice always arises from a collaborative decision-making process involving the patient, the dermatologist, and sometimes, an oncologist.
Navigating the journey of non-melanoma skin cancer treatment requires informed choices, trust in healthcare providers, and the resilience to move forward with a chosen strategy. But with evolving medical advancements and a patient-centric approach, many find their way to recovery and healing.
Surgical Procedures
Surgical excision involves removing the tumor and a margin of healthy skin around it. It’s a common method for treating non-melanoma skin cancers.
Mohs surgery is a specialized procedure where thin layers of cancer-containing skin are progressively removed and examined until only cancer-free tissue remains.
Non-Surgical Treatments
Topical treatments involve applying creams or gels directly to the tumor. They’re best suited for superficial cancers.
Cryotherapy uses extreme cold to freeze and destroy cancer cells. It’s a quick procedure but might require multiple sessions.
Superficial Radiotherapy
Superficial radiotherapy stands out as a specialized form of radiation therapy tailored explicitly for skin cancers. Unlike traditional radiation therapies that penetrate deep into the body, superficial radiotherapy employs low-energy X-rays. These X-rays are meticulously calibrated to target only the cancerous cells on the skin’s surface, ensuring that the deeper, healthy tissues remain unaffected. This precision not only ensures effective treatment but also minimizes potential damage to the surrounding areas.
Benefits
When it comes to treating skin cancers, especially those in challenging or sensitive locations, superficial radiotherapy presents a compelling alternative to surgical interventions. One of its most significant advantages is its non-invasive nature. Unlike surgeries that involve incisions and can sometimes lead to complications, superficial radiotherapy is administered externally. This means patients don’t have to worry about prolonged recovery times or potential infections. Moreover, because there’s no cutting involved, the treatment significantly reduces the risk of leaving behind any unsightly scars, ensuring that the skin retains its natural appearance as much as possible.
Procedure and Aftercare
Undergoing superficial radiotherapy is a systematic process that requires commitment from the patient. Typically, the treatment is spread out over multiple sessions spanning several weeks. This phased approach ensures that the maximum number of cancer cells are targeted and destroyed. After each session, it’s not uncommon for patients to notice some changes in the treated skin area. The skin might take on a reddish hue or become slightly swollen. Some patients might even experience a mild burning sensation. However, it’s crucial to understand that these side effects are a natural part of the healing process and are generally temporary. With proper aftercare, which may include moisturizing creams and avoiding direct sunlight, these symptoms usually subside within a few days. Regular follow-ups with the healthcare provider are also essential to monitor the skin’s response to the treatment and make any necessary adjustments.
Factors to Consider
When deciding on a treatment, consider the type and stage of the cancer, its location, potential side effects, and your personal preferences. Always consult with a dermatologist or oncologist to make an informed decision.
Conclusion
Though non-melanoma skin cancer is typically not as aggressive as melanoma, it’s imperative to address it swiftly and efficiently. A plethora of treatments, spanning from surgical interventions to less invasive methods, provides patients with a diverse array of choices. Notably, superficial radiotherapy stands out as a technique that minimizes invasiveness and scarring. Engaging in a thorough conversation with a medical expert is crucial to pinpoint the most suitable treatment tailored to an individual’s unique situation.
Follow me down the rabbit hole!
I'm Alice and I live with a dizzying assortment of invisible disabilities, including ADHD and fibromyalgia. I write to raise awareness and end the stigma surrounding mental and chronic illnesses of all kinds.